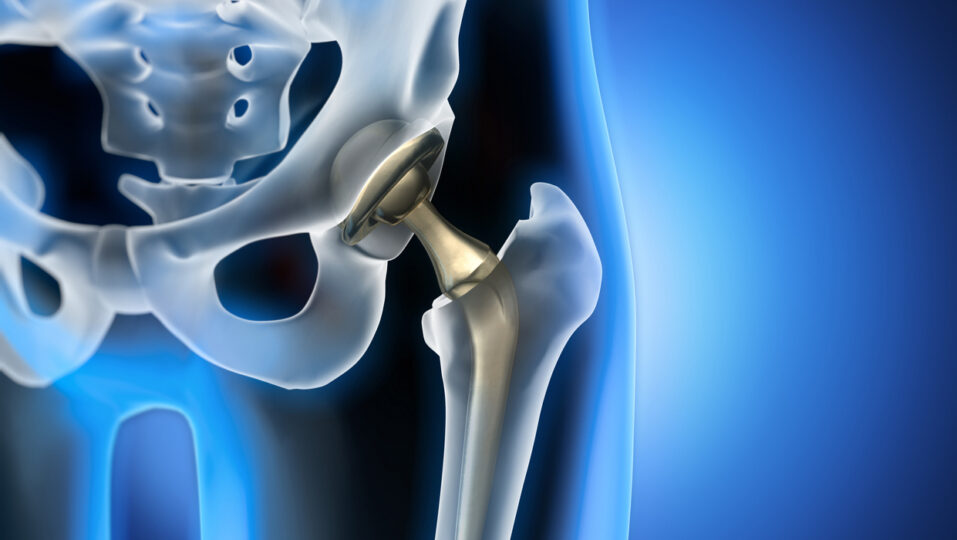
Hip replacement surgery is not only one of the most commonly performed orthopedic surgeries today, but it is also one of the most successful. If you suffer from the daily pain and loss of mobility from hip arthritis, you can look forward to enjoying a fuller, healthier, and more active life after having hip replacement surgery.
Let’s talk about what you can expect your recovery to be like during the first year after having hip replacement surgery, and where you can go in Raleigh for expert orthopedic consultation and treatment that greatly reduces or eliminates your hip pain for good.
The First Few Days After Hip Surgery
Immediately after hip replacement surgery, you can expect to be given pain medication either through your IV, by mouth, or both. You will also be given antibiotics to prevent infection and blood thinners to prevent blood clots.
Physical therapy will begin right away, often later the same day when you had the operation. You will be taught how to walk with an assistive device, like a walker, which can be used until you gain more strength and balance. This early movement will help to restore normal hip function and to prevent complications such as blood clots.
After you have practiced walking and are now walking around comfortably with a walker, you will also learn rehabilitative exercises and practice going up and downstairs. These exercises should typically be done two to three times daily for 20 to 30 minutes per session. These exercises will also help to restore the normal function of your hip, as well as improve its strength and range of motion.
In addition, you will be advised to avoid performing certain movements in order to protect your new hip. You should not twist or pivot on your surgical leg, avoid bending your hip more than 90 degrees either by squatting or bending over and do not cross your leg over the midline of your body or twist it in an inward rotation. This a safe framework to follow in the beginning to protect the new hip while it heals.
The First Few Weeks of Recovery
Your first few weeks after hip replacement surgery will be dedicated to preventing complications, promoting healing, and improving the strength and mobility of your new hip. You will begin an outpatient physical therapy program to guide you through the recovery process.
A tailored exercise program will be developed specifically for you by your physical therapist with input from your orthopedic surgeon. Your successful rehabilitation depends on you following your planned exercises and stretches as recommended. Do your exercises regularly, and be sure to keep all of your follow-up appointments and physical therapy sessions. Your therapist will help guide the transition from using a walker to a cane and then walking without any assistance, which typically occurs over the first few weeks after surgery.
You will be given pain medication, and you should take it if needed, but most patients require very few if any pain pills after surgery. Blood clots are a potential but rare complication after hip replacement surgery, so it is important that you take any blood thinners exactly as directed. Be aware of any signs of a blood clot, including leg swelling (with or without pain), shortness of breath, or chest pain. If you experience any of these symptoms, call 911 or go to the emergency room.
While your surgical wound is still healing, be sure to keep your dressings dry and follow any instructions for incision care that are given to you. If you develop a fever of over 101.5 degrees or experience increased (rather than reduced) drainage, swelling, or pain while you’re healing, call your surgeon.
Be sure that any tripping hazards are removed around the house; ask someone else for help with this if necessary. A healthy diet and good nutrition will also promote your healing.
The First Few Months of Hip Replacement Recuperation
The first several months after hip replacement surgery are very important to your long-term health and increased mobility. In fact, while you may see continued improvement for up to a year, you should expect to return to many normal activities within two or three months or less – such as driving, working, shopping, and doing errands.
By the end of the first three months after your hip operation, your hip pain should be minimal to none; however, you will continue to be monitored for complications and healing. Preventing a fall is paramount. Wear well-fitting shoes that do not have open backs, pay attention to your surroundings and any potential hazards, make sure that your eyesight is corrected if you have any vision problems, and always make sure there is adequate lighting when moving about. Confidence while walking is a great way to prevent falls.
Twelve Months Out and Beyond
While most of your recovery will be completed within the first few months after your hip replacement surgery, you will continue to enjoy improvement throughout the first year as you get stronger. Your surgeon will advise you against any high-impact activities, such as running, but low-impact and no-impact physical activity (such as walking and swimming) is encouraged. Patients typically return to activities such as golf, tennis, and hiking, and many others.
Hip Replacement Surgeon in Raleigh
If you have hip arthritis or chronic hip pain, our friendly team is here to answer any questions you have. To seek the expert advice of experienced orthopedic surgeon Dr. Brett Gilbert, contact us today by calling us at (919) 788-8797 or you can request an appointment with Dr. Gilbert using our appointment request form, or you can self-schedule your appointment here.
Our goal is to help you get back on the road to a pain-free and healthy lifestyle!